During exercise, active muscles require more oxygen. More nutrients are required, and as metabolism increases, more waste is created. Body temperature may also increase, and with intense exercise, as lactic acid builds up, the concentration of hydrogen ions (H+) in muscle and blood increases, lowering their pH. Changes that occur in the CVS during exercise are designed to meet these increased demands, and counter-balance the consequences, so that the system can continue to work efficiently whilst maintaining normal body temperature and pH. (ie maintaining homeostasis). The most significant changes in the CVS during exercise include changes in heart rate; stroke volume; cardiac output; blood flow; blood pressure; and the blood.
|
Heart Rate
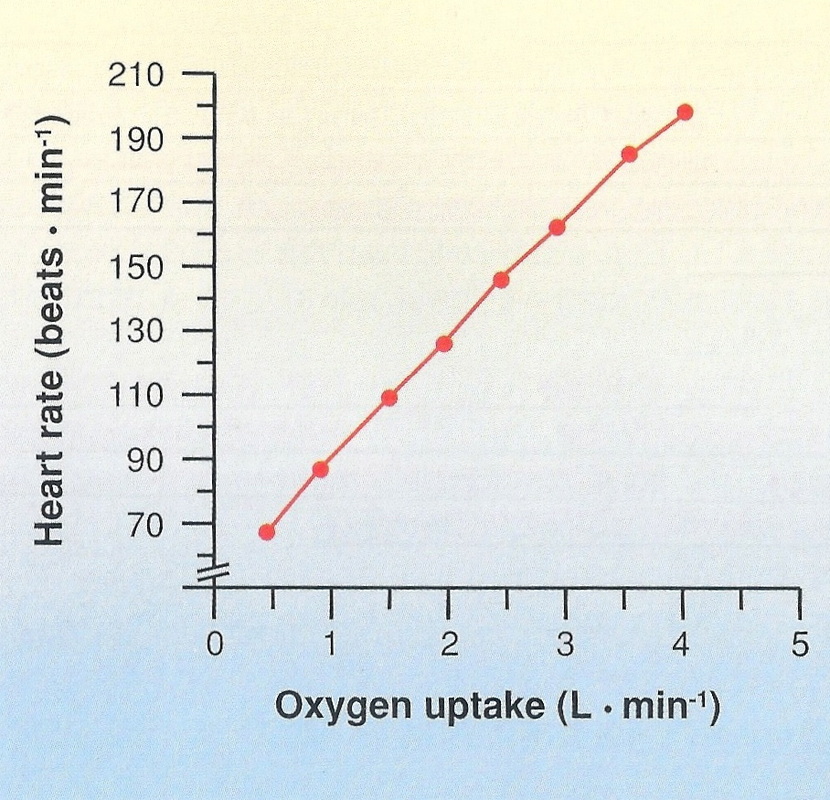
Your heart rate is the number of beats your heart takes in one minute. The average resting heart rate for an adult is between 60-80 beats per minute, but ranges greatly. Resting heart rate usually decreases with age, and is affected by environmental factors such as temperature and altitude. Prior to commencing exercise, your heart rate starts to climb significantly above the resting rate in anticipation of the increased demands of the body. This is controlled through the autonomic nervous system by chemicals such as adrenaline. When exercise starts, your heart rate increases rapidly in direct proportion to your exercise intensity (and how much oxygen your body requires for the activity). As exercise continues, the build-up of lactic acid, increased heat formed as a result of increased muscular activity, and the production of more carbon dioxide all stimulate further increases in heart rate, until you are near the point of exhaustion. At this point you are approaching your maximal heart rate (HRmax). This is the highest heart rate you can achieve in an all-out effort to exhaustion. Your HRmax is relatively constant, changing only with your age. It can be estimated by subtracting your age from 220.
When exercise levels are held constant, the heart rate increases fairly rapidly to meet the demands of this exercise, and then plateaus at this level. This is known as the steady state heart rate. For each increase in intensity, the heart rate increases to a new steady-state value, and the more intense the exercise, the longer it will take the heart to reach this new level. |
Stroke Volume
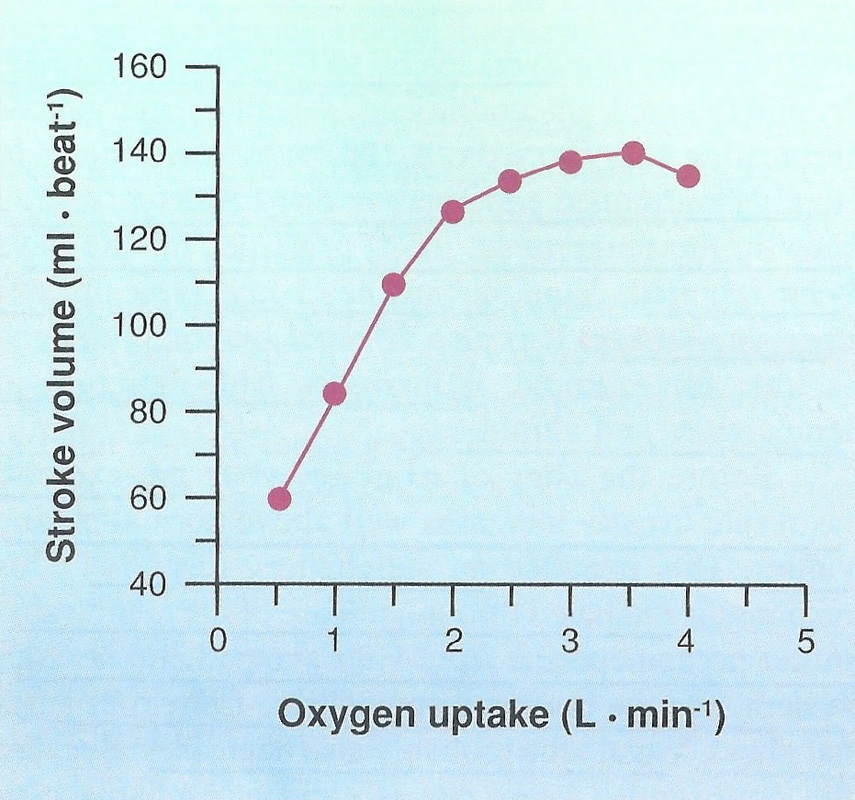
The stroke volume is the amount of blood ejected from the left ventricle in a single contraction. It is dependent on how much blood returns to the heart from the veins, how much the ventricle can distend, and then contract, and the pressure against which it must contract. The average resting stroke volume for an adult is approximately 60mL. During exercise, the stroke volume increases with increasing rates of work, but only up to an exercise intensity between 40-60% of maximum. Beyond this, the stroke volume plateaus. The increase in SV is usually a combination of more blood returning to the heart, greater distention of the ventricle, and then greater contraction of the ventricle. More blood returns to the heart (venous return) as a result of both the skeletal muscle pump and respiratory pumps.
The plateau seen, as heart rates approach maximum is probably best explained by a shorter resting phase of the heart (diastole), giving the chamber less time to fill, and therefore the distention of the ventricle will taper off. |
Cardiac Output
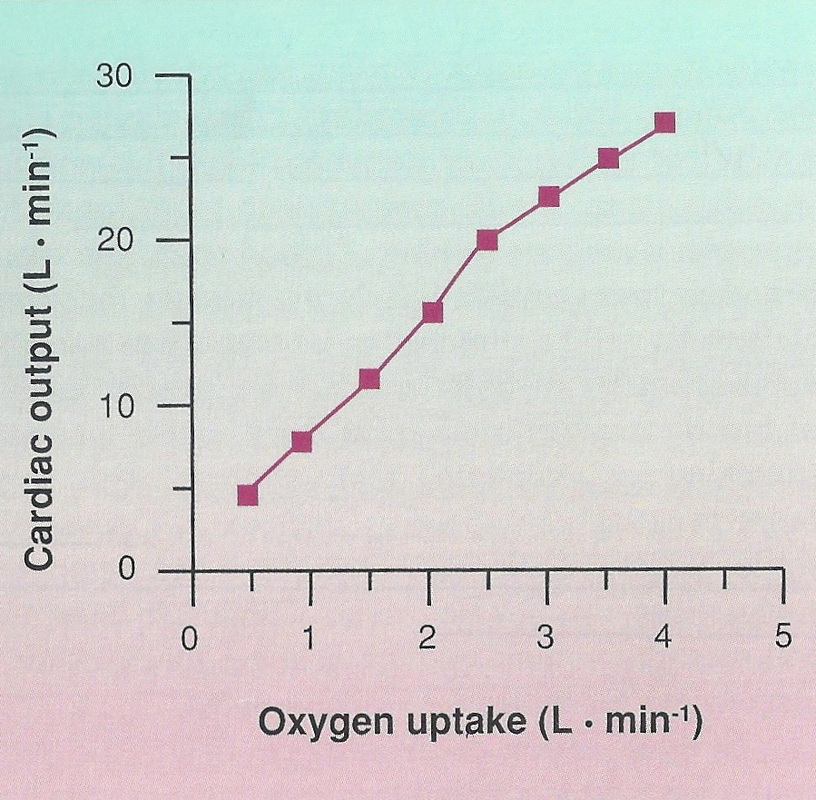
The cardiac output (Q) is the total volume of blood pumped by the left ventricle per minute. It is calculated by multiplying the heart rate (HR) by the stroke volume (SV). Q=HRxSV Given that both heart rate and stroke volume increase with exercise, it is easy to deduce that cardiac output will increase with increasing intensity of exercise. The average resting cardiac output for an adult is around 5.0L/min (average heart rate around 80 and average stroke volume around 60mL). cardiac output increases directly with increasing exercise intensity to levels around 20-40L/min, depending on body size and how fit you are.
During the early stages of exercise, the increased cardiac output is a result of increases in both stroke volume and heart rate. However, as exercise intensity climbs to levels greater than 40-60% maximal capacity, any increases are largely due to increases in heart rate, as the stroke volume has plateaued. The increase in cardiac output contributes to an increase in blood returning to the heart, which in turn increases the cardiac output. |
|
Blood Flow
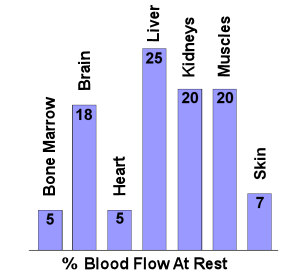
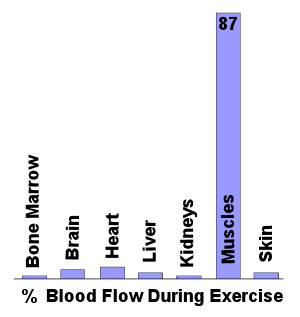
The vascular system has the ability to redistribute blood to the areas with the greatest need for oxygen and nutrients, whilst reducing the flow to areas where the requirements are not as great. At rest, approximately 15% of the cardiac output goes to muscle, but this increases to around 85% with intense exercise. This occurs largely because of reduced blood flow to organs such as the stomach and intestines during exercise. As we start to exercise, our muscles require more oxygen for increased metabolism, and as exercise continues, acid and CO2 build up and must be taken away to perform efficiently. Blood flow is diverted by the constriction of vessels to the organs with low need (liver, kidneys, stomach, intestines, etc), and dilatation of the vessels where blood flow must increase (muscles). As the muscles work, more heat is also generated, and this too must be dissipated. Blood flow therefore also increases to the skin so heat can be released.
|
Blood Pressure
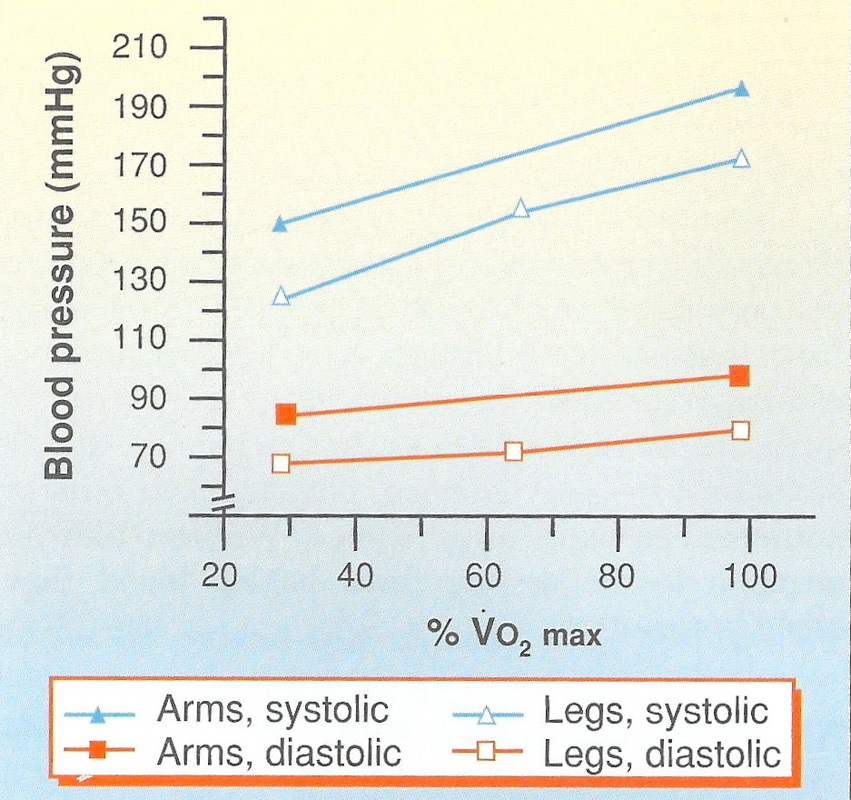
Blood pressure is expressed by two numbers. The systolic pressure, or higher number, is the highest pressure in the artery, and corresponds to the pressure in the vessel as the ventricle contracts (systole). The diastolic pressure is the lower number and represents the lowest pressure in the artery, when the ventricle is at rest (diastole). With endurance exercise, the systolic blood pressure increases in direct proportion to increased exercise intensity. A normal systolic blood pressure is approximately 120mmHg. This can climb to 250mmHg in normal, healthy, highly trained athletes during high intensity exercise. This increase helps to drive blood quickly through the vessels, and forces blood through the capillaries faster, facilitating the delivery of oxygen and nutrients. In contrast, the diastolic pressure does not change very much during exercise, regardless of the intensity. None of the changes seen in the cardiovascular system effect the heart in the resting phase, and therefore the diastolic pressure should be relatively unchanged. Blood pressure response to resistance exercise, such as weightlifting, is incredible. Levels of 480/350mmHg have been measured in weightlifters. This is due to the exertion phase of a lift, where the lifter attempts to exhale with the mouth, nose and glottis closed, creating huge pressure in the chest cavity which the body must overcome.
|
The Blood
At rest, the bloods oxygen content varies from 20mL oxygen in 100mL arterial blood, to approximately 14mL oxygen in 100mL venous blood. The difference is 6mL and this represents how much oxygen has been extracted by working tissues and organs. As we exercise, the working muscles begin to extract more oxygen, so this difference increases. In fact, the venous oxygen content in working muscles is often close to zero. This means blood returning to the heart has significantly reduced oxygen levels, so when it reaches the capillaries next to alveolae, the diffusion of oxygen into the blood is increased. With exercise, the plasma volume (fluid portion of the blood) can quickly decrease as fluid is lost into the spaces between vessels. This is largely due to an increase in blood pressure, which forces fluid out of the capillaries. A 10-20% reduction in plasma volume is not uncommon with prolonged work. This can be exacerbated by hot environmental conditions. A reduction in plasma volume can impair performance as blood flow can ultimately be reduced. This is why rehydration during prolonged exercise is so important. As the plasma volume decreases, the cellular component increases its ratio (ie the haematocrit increases). The red cells contain haemoglobin, which carries the oxygen in the blood. This increase in haematocrit, increases the oxygen carrying capacity of blood. However, this may be offset by the reduction in plasma volume, which can increase the viscosity of blood, reducing the blood flow. At rest, arterial blood pH is approximately 7.4 (slightly alkaline). This does not change much up to exercise intensity of approximately 50% aerobic maximum. At levels beyond 50%, lactic acid starts to build up as there is a switch from aerobic to anaerobic metabolism. This results in a fall of blood pH to as low as 6.5 in active muscles during sprint-type activities. |